On the surface, psoriasis looks like a skin problem. Red patches. Silvery scales. Dry, itchy areas that refuse to heal.
But beneath those visible symptoms lies a much deeper story — one that involves the immune system, genetics, inflammation, and the complex relationship between lifestyle and health.
For millions of people around the world, psoriasis is not just a cosmetic concern. It is a lifelong autoimmune condition that can affect physical comfort, emotional well-being, and sometimes even the joints and internal organs.
Understanding psoriasis is the first step toward managing it effectively.
 What Is Psoriasis?
What Is Psoriasis?
Psoriasis is a chronic autoimmune inflammatory disease that primarily affects the skin.
Normally, skin cells grow and shed in a cycle that takes about 28–30 days. In people with psoriasis, the immune system mistakenly accelerates this process, causing skin cells to multiply up to 10 times faster than normal.
Instead of shedding naturally, the extra skin cells pile up on the surface, forming thick, red patches covered with silvery scales known as plaques.
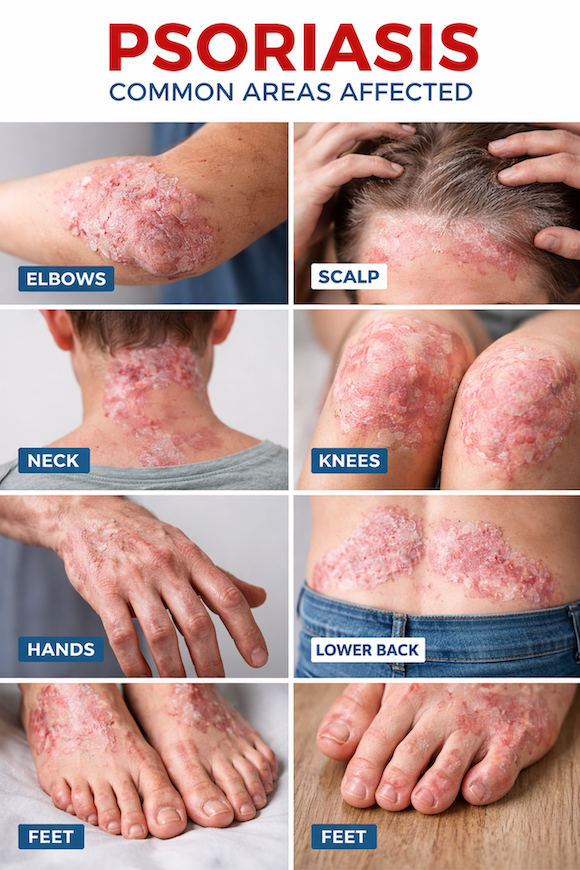
These plaques most commonly appear on:
- Elbows
- Knees
- Scalp
- Lower back
- Hands and feet
In some cases, psoriasis can also affect nails, joints, and other parts of the body.
How Common Is Psoriasis?
Psoriasis is one of the most common autoimmune diseases worldwide.
Global estimates suggest:
- About 2–3% of the world’s population lives with psoriasis
- Roughly 125 million people worldwide are affected
- About 7.5 million people in the United States have psoriasis
The condition affects men and women equally.
However, prevalence varies across populations.
Higher rates are found in:
- Northern Europe
- Scandinavia
- North America
Lower rates are seen in:
- East Asia
- Indigenous populations
- Some African regions
Genetics appear to play a major role. People with a family history of psoriasis are significantly more likely to develop it.
Common Symptoms
Psoriasis symptoms vary widely depending on the type and severity, but the most common signs include:
Skin Symptoms
- Thick red patches of skin (plaques)
- Silvery-white scales
- Dry or cracked skin that may bleed
- Intense itching or burning sensation
Nail Changes
- Pitting in fingernails
- Thickened nails
- Nail separation from nail bed
Scalp Symptoms
- Flaky patches that resemble severe dandruff
- Thick plaques extending beyond the hairline
Other Symptoms
- Skin pain or tenderness
- Stiff or swollen joints in some patients
Symptoms often occur in cycles, with flare-ups followed by periods of remission.
Types of Psoriasis
Dermatologists typically classify psoriasis into several forms:
Plaque Psoriasis
The most common type, accounting for 80–90% of cases.
Characterized by raised red patches covered with silvery scales.
Guttate Psoriasis
Often triggered by bacterial infections such as strep throat, especially in children or young adults.
Appears as small drop-shaped spots.
Inverse Psoriasis
Occurs in skin folds such as under the breasts, groin, or armpits.
Lesions appear smooth and shiny rather than scaly.
Pustular Psoriasis
Produces white pus-filled blisters surrounded by red skin.
Erythrodermic Psoriasis
A rare but severe form that causes widespread redness and inflammation across most of the body.
This type may require emergency medical care.
Which Age Groups Are Most Affected?
Psoriasis can appear at any age, but two peaks are most common:
First peak:
Age 15–35
Second peak:
Age 50–60
However, children, middle-aged adults, and older individuals can all develop the condition.
Some people experience psoriasis for decades with periods of remission and flare-ups.
What Causes Psoriasis?
The exact cause is not fully understood, but psoriasis develops from a combination of three major factors:
1. Immune System Dysfunction
The immune system mistakenly attacks healthy skin cells, triggering inflammation.
2. Genetics
About one-third of patients have a family history of psoriasis.
Researchers have identified multiple genes associated with the condition.
3. Environmental Triggers
External factors can trigger flare-ups.
Common triggers include:
- Stress
- Skin injuries or cuts
- Infections
- Cold weather
- Certain medications
Can Medications Trigger Psoriasis?
Yes. Some medications are known to worsen or trigger psoriasis in susceptible individuals.
These include:
- Lithium (for bipolar disorder)
- Beta blockers (for heart conditions)
- Antimalarial drugs
- Interferons
- Rapid withdrawal of corticosteroids
If psoriasis symptoms appear after starting a medication, patients should consult their physician before stopping treatment.
Lifestyle Factors That Influence Psoriasis
Lifestyle plays a significant role in controlling flare-ups.
Factors that may worsen psoriasis include:
- Smoking
- Heavy alcohol consumption
- Chronic stress
- Obesity
- Lack of sleep
Conversely, healthier habits can significantly improve symptoms.
Foods and Drinks That May Trigger Flare-Ups
Although psoriasis is not strictly a diet-related disease, certain foods appear to worsen inflammation in some people.
Common triggers include:
Foods that may worsen symptoms
- Processed foods
- High sugar intake
- Red meat
- Fried foods
- Refined carbohydrates
- Alcohol
Potentially helpful foods
- Fatty fish rich in omega-3 (salmon, sardines)
- Leafy green vegetables
- Fruits rich in antioxidants
- Whole grains
- Nuts and seeds
- Olive oil
An anti-inflammatory diet similar to the Mediterranean diet may help reduce flare-ups.
Can Psoriasis Be Linked to Other Diseases?
Research increasingly shows that psoriasis is not just a skin condition.
It is associated with systemic inflammation and may increase the risk of several health problems.
These include:
- Psoriatic arthritis
- Heart disease
- Metabolic syndrome
- Type 2 diabetes
- Obesity
- Depression and anxiety
Because of these links, dermatologists now often recommend a whole-body health approach when treating psoriasis.
 Psoriasis vs. Psoriatic Arthritis
Psoriasis vs. Psoriatic Arthritis
About 30% of people with psoriasis eventually develop psoriatic arthritis, a form of inflammatory arthritis.
Key differences include:
| Feature | Psoriasis | Psoriatic Arthritis |
|---|---|---|
| Primary symptom | Skin plaques | Joint pain and swelling |
| Areas affected | Skin and scalp | Joints, tendons, ligaments |
| Nail changes | Common | Common |
| Joint stiffness | Rare | Common |
| Morning stiffness | Rare | Often present |
Symptoms of psoriatic arthritis may include:
- Swollen fingers or toes
- Joint pain and stiffness
- Reduced mobility
- Back pain
Early diagnosis is important because untreated psoriatic arthritis can cause permanent joint damage.
Treatments for Psoriasis
While psoriasis cannot yet be permanently cured, modern treatments can control symptoms extremely well.
Treatment options include:
Topical Treatments
Used for mild cases.
Examples include:
- Corticosteroid creams
- Vitamin D analogs
- Coal tar preparations
- Salicylic acid
Phototherapy
Controlled exposure to ultraviolet light can slow skin cell growth.
Systemic Medications
Used for moderate to severe psoriasis.
These include:
- Methotrexate
- Cyclosporine
- Oral retinoids
Biologic Therapies
One of the most significant advances in modern dermatology.
Biologics target specific immune pathways responsible for inflammation.
Many patients achieve near-complete skin clearance with these treatments.
Preventing Psoriasis Flare-Ups
Although psoriasis cannot always be prevented, flare-ups can often be minimized.
Helpful strategies include:
- Managing stress
- Maintaining a healthy weight
- Avoiding smoking
- Limiting alcohol intake
- Protecting skin from injury
- Treating infections promptly
- Following a balanced anti-inflammatory diet
Keeping the skin well moisturized is also important.
The Emotional Side of Psoriasis
Because psoriasis affects visible parts of the body, many patients experience emotional challenges such as:
- Low self-esteem
- Social anxiety
- Depression
Support groups, counseling, and education can be valuable components of long-term management.
Increasing awareness has helped reduce stigma surrounding the condition.
Is There a Cure?
At present, there is no permanent cure for psoriasis.
However, modern medicine has made remarkable progress.
Many people today can achieve long periods of remission and near-normal skin with the right treatment plan.
The future is promising. Researchers are actively exploring:
- Advanced biologic therapies
- Genetic research
- Immune system modulation
These developments may eventually lead to more definitive treatments.
Final Thoughts
Psoriasis reminds us that the body is deeply interconnected. What appears on the skin often reflects complex processes within the immune system.
With proper diagnosis, lifestyle adjustments, and modern treatments, most people with psoriasis can lead healthy, active, and fulfilling lives.
Understanding the condition — and recognizing early symptoms — empowers individuals to take control of their health.
-Nguyễn Duy Khiêm-
Sources for Further Reading
American Academy of Dermatology
https://www.aad.org
National Psoriasis Foundation
https://www.psoriasis.org
National Institutes of Health
https://www.nih.gov
Mayo Clinic
https://www.mayoclinic.org
World Health Organization – Psoriasis Global Report
https://www.who.int
Harvard Medical School – Skin Disease Research
https://www.health.harvard.edu
